On the International Space Station 220 miles above the earth, a microAnalyzerTM monitors air quality with extreme precision to ensure astronauts aren’t breathing in hazardous chemicals.
At Brigham and Women’s Hospital (BWH) in Boston, this same shoebox-sized instrument is helping diagnose pneumonia, thanks to the curiosity of Sophia Koo, MD, a specialist in infectious diseases. Koo treats people whose weakened immune systems make them susceptible to pneumonia and other infections. One in four of her patients with aspergillosis, a dangerous fungal pneumonia, die of this infection.
“Diagnostic tests for pneumonia using blood samples, lung washings, or lung biopsies are slow, invasive, and inaccurate,” says Koo. Her frustration led her to wonder if aspergillosis could be detected in a person’s breath.
“Most people have at least 100 to 200 chemicals in their breath,” Koo says. “When you have pneumonia from a bug that is not supposed to be growing in your lung, chemicals can show up that are not usually there. This is true for aspergillosis.”
Koo learned that the inventor of the microAnalyzer™, Cambridge-based Draper Laboratory, was interested in medical uses for this chemical detection tool. Koo and scientists at Draper began collaborating on a breath-based diagnostic test for pneumonia that can yield precise results within minutes—not the days or weeks typical of existing approaches. They plan to seek approval from the U.S. Food and Drug Administration, so the clinical microAnalyzer™ can be used to diagnose pneumonia and other infectious diseases in medical settings across the country.

Clinically Motivated
Koo’s work shows how scientific curiosity can lead to improved patient care, and vice versa. A concept known as translational research, physician-scientists translate discoveries in the lab into new treatments and devices for patients, while observing trends in the clinic that inform their research.
“Translational research is the dedication to ensuring that scientific findings are made relevant to patient care,” says Elazer Edelman, MD, PhD. “The ideas we pursue are pushed from behind by clinical need and pulled from the front by clinical use.”
Edelman runs several research centers at BWH, Harvard Medical School, and the Massachusetts Institute of Technology that combine engineering, science, biology, and physiology to improve the quality of people’s lives. A senior attending physician in BWH’s coronary care unit, Edelman draws his research inspiration from his patients.
“The patients drive what we investigate, and what we investigate drives our practice of medicine,” he says. “For example, we gained a greater understanding of blood vessel health through research, and used this knowledge to create new cell-based therapies and devices—including stents, heart valves, and ventricular assist devices.”
Translational research is the dedication to ensuring that scientific findings are made relevant to patient care. The ideas we pursue are pushed from behind by clinical need and pulled from the front by clinical use.
Elazer Edelman, MD, PhD
Creating an environment that supports complex translational research is a top priority at BWH, according to Chief Academic Officer and Senior Vice President of Research Paul Anderson, MD, PhD.
“Turning research into remedies is no easy task,” Anderson says. “As an institution, we’re seeking new ways to give our researchers and clinicians more opportunities to work together and bring their ideas to life.”
Building Collaboration
Recently opened in October, the hospital’s Building for Transformative Medicine is designed to help overcome obstacles to translational research. It houses medical specialties such as the neurosciences, orthopaedics, rheumatology, and immunology.
“Allowing seemingly disparate teams to now work side by side is a beautiful feature of the new building,” says Tanya Laidlaw, MD, director of translational research in allergy and immunology. “Epidemiologists, geneticists, animal model specialists, and clinicians can collaborate more easily.”
Laidlaw specializes in caring for people with aspirin-exacerbated respiratory disease (AERD). “We recently discovered that roughly 80 percent of our patients with AERD develop respiratory reactions related to alcohol,” she says, noting that a glass of wine or beer can cause congestion, sneezing, wheezing, and asthma in these individuals. “This phenomenon confounds doctors because most clinics don’t have enough patients with this disease to notice the pattern and ask the questions. But we do.”
To improve medicine, there must be a constant back and forth of information between lab investigations and patient care.
Tanya Laidlaw, MD
Informed by their observations in more than 200 patients, Laidlaw and her colleagues are now collaborating to explore the cause of these respiratory reactions to alcohol.
“To improve medicine, there must be a constant back and forth of information between scientific investigations and patient care,” she says. “The Building for Transformative Medicine facilitates that ongoing exchange.”
The Science of Startups
The new building also strengthens BWH’s existing translational research tools. For example, it now houses the Brigham Innovation Hub (iHub), a resource center that helps BWH innovators turn their ideas and inventions into medical services and products that benefit patients. Established in 2013, iHub offers brainstorming sessions and healthcare business workshops, and links researchers with people from a range of fields who can help investigators to move their projects forward.

One spring morning last year, Alexander Lin, PhD, took the podium at an iHub pitch session to share his idea for a software platform to make complex brain imaging easier.
“It was different from anything I’d experienced before,” recalls Lin, director of the Center for Clinical Spectroscopy at BWH. “My medical colleagues were there, along with graphic designers, businesspeople, programmers, and engineers.”
At the pitch session, Lin and four of his colleagues presented their ideas to a panel of BWH medical experts, while specialists from other fields sketched out product mockups and shared business development advice in real time.
Ultimately, iHub granted Lin’s team $20,000 to help develop his software platform and offered ongoing guidance related to marketing, regulatory requirements, patents, and entrepreneurship. Six months later, Lin’s idea blossomed into a startup company called BrainSpec.
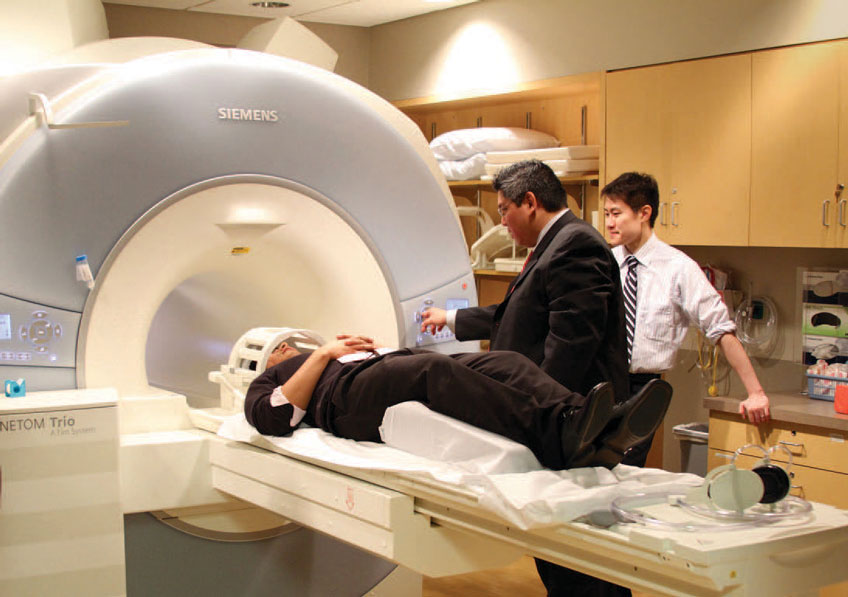
“Our software cuts data processing time from three days to just 30 seconds,” Lin says. “It also allows anyone on the clinical staff to reconstruct the spectroscopy data, rather than the current method, which involves a physicist.”
Lin first came up with this concept 15 years ago. “I had been batting this idea around for so long, trying to figure out how to make it a reality,” he says. “BrainSpec happened because iHub provided the resources and know-how to make it happen.”
Minding The Gap
Lin’s long road to BrainSpec illustrates one of translational medicine’s biggest hurdles: the time it takes for new medical solutions to reach patients. Through the Building for Transformative Medicine, Brigham Innovation Hub, and other new initiatives, BWH hopes to shorten this time frame, says Allison Moriarty, vice president of research administration and compliance.
“In translational research, there’s always a gap between developing a new treatment or technology, testing it in animal models, testing it in humans, and then getting it to patients,” she says. “We’re looking at how to expedite what’s happening preclinically so that we can translate it into an effective medical product or clinical care.”
The latest efforts include creating a specialized infrastructure to bring the most promising research into early-phase clinical trials—studies that test treatments in patients for the first time (see “Approaching Truth”).
“Not every lab discovery translates into technology or practice, so there is a lot we can do to help evaluate different therapies,” Moriarty says. “The work we’re doing will help determine which therapies should make that leap into clinical trials— which are the most likely to be successful—and then accelerate those in the hopes of new treatments reaching patients faster.”